Transmission
Animal bites, non-bite exposure, or human-to-human exposure are all ways in which rabies can be transmitted. In most cases, transmission of the virus is caused by the bite of a rabid animal. Rabies cannot be spread through casual contact, such as touching a person with the disease, or contact with noninfectious fluid or tissue.
How Is Rabies Transmitted?Rabies transmission can occur in one of a few ways, including:
A bite from a rabid animal (an animal infected with the rabies virus) is the most common form of rabies transmission. Non-bite exposure and human-to-human exposure are both rare. Rabies Transmission from Bites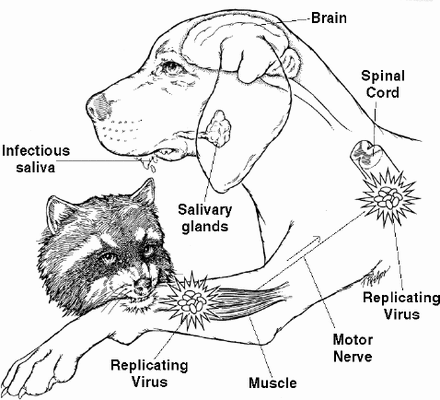
The rabies virus attacks nervous tissue and appears to replicate almost exclusively in neuronal cells. Once introduced through the skin or mucous membrane, the virus begins replicating in the striated muscles at the wound site. The virus can replicate in muscle cells for hours or weeks, or it can migrate immediately to the nervous system via unmyelinated sensory nerve endings at the inoculation site.
Migration to the nervous system is via the nearest sensory or motor neuron in the ganglion at the base of the spinal cord or to the spinal cord itself. Once there, the virus continues to replicate. (It can then be transported back to the wound site or up to the brain via the central nervous system.) Axonal transport to the CNS is at a rate of 3 mm per hour. It is possible however, that the virus also moves across cell-to-cell junctions, and not just among nerve trunks. In the brain, the virus infects neurons in almost all brain regions, where it continues replication. Neuronal virus transmission from the periphery of the body to the brain is called "centripetal virus spread." Possible receptors for the virus are: acetylcholine receptors, gangliosides, and phospholipids. In aerosol transmission, the virus enters the body through the nasal epithelium and is subsequently transported to the olfactory bulb. It is thought that the virus replicates in the neurons of the olfactory bulb before spreading to other neurons in the brain. After the rabies virus infects the brain, it can continue to spread throughout the body via efferent neural pathways. At this stage, the virus can be found in salivary glands, taste buds, nasal cavities, tears, skin, the adrenal glands, pancreas, kidney, heart muscle, brown fat, hair follicles, retina, and cornea. (The virus has never been detected in blood or blood cells.) Additional notes: • Neurological research has suggested that death from rabies is not a result of structural damage caused by the virus, but rather a result of functionalalteration of neurons. The rabies RNA most likely competes with host RNA, impairing neural functions. Neurologic damage is exacerbated by the production of certain cytokines, such as tumor necrosis factor-alpha. In addition, the body's own immune response to rabies includes the production of nitric oxide, which may act as a toxin to the CNS. • One of the determining factors of rabies virulence is the glycoprotein (GP) which makes up the viral membrane. In particular, the amino acid site at position 333 seems to be critical to pathogenicity. Argine or lysine residues at this site seem to confer virulence. Substituting different amino acids at this position resulted in viruses which were attenuated. The attenuated viruses spread more slowly in the CNS and do not seem able to infect certain types of nerve fibers. Reverting to the original amino acid (arginine) at the site restores neurovirulence. Reference:http://www.tarakharper.com/v_rabies.htm |
Rabies transmission Through Non-Bit
Rabies transmission from non-bite exposures is rare. Scratches, abrasions, open wounds, or mucous membranes contaminated with saliva or other potentially infectious material (such as brain tissue) from a rabid animal, constitute non-bite exposures. Occasionally reports of non-bite exposure are such that post-exposure prophylaxis is given.
Inhalation of aerosolized rabies virus is also a potential non-bite route of exposure, but with the exception of laboratory workers, most people are unlikely to encounter an aerosol version of the rabies virus.
Other contact, such as petting a rabid animal, or contact with the blood, urine, or feces (e.g., guano) of a rabid animal, does not constitute an exposure and is not an indication for prophylaxis.
Reference:-http://rabies.emedtv.com/rabies/rabies-transmission.html
Inhalation of aerosolized rabies virus is also a potential non-bite route of exposure, but with the exception of laboratory workers, most people are unlikely to encounter an aerosol version of the rabies virus.
Other contact, such as petting a rabid animal, or contact with the blood, urine, or feces (e.g., guano) of a rabid animal, does not constitute an exposure and is not an indication for prophylaxis.
Reference:-http://rabies.emedtv.com/rabies/rabies-transmission.html
Human-to-Human Rabies Transmission
Rabies transmission between humans is also extremely rare. The only well-documented cases of rabies caused by human-to-human transmission occurred among eight recipients of transplanted corneas, and recently among three recipients of solid organs. Guidelines for acceptance of suitable cornea and organ donations, as well as the rarity of human rabies in the United States, have reduced the risk of rabies transmission occurring through transplanted organs.
In addition to rabies transmission from cornea and organ transplants, bite and non-bite exposures inflicted by infected humans could theoretically transmit rabies, but no such cases have been documented.
Rabies transmission cannot occur through casual contact, such as touching a person with rabies or contact with non-infectious fluid or tissue (e.g., urine, blood, or feces). In addition, contact with someone who is receiving the rabies vaccination does not constitute rabies exposure and does not require post-exposure prophylaxis.
In addition to rabies transmission from cornea and organ transplants, bite and non-bite exposures inflicted by infected humans could theoretically transmit rabies, but no such cases have been documented.
Rabies transmission cannot occur through casual contact, such as touching a person with rabies or contact with non-infectious fluid or tissue (e.g., urine, blood, or feces). In addition, contact with someone who is receiving the rabies vaccination does not constitute rabies exposure and does not require post-exposure prophylaxis.
The Path of the Virus
1.The Virus Travels Through the Body
From numerous studies conducted on rabid dogs, cats, and ferrets, we know that when the rabies virus is introduced into a muscle through a bite from another animal, it travels from the site of the bite to the brain by moving within nerves. The animal does not appear ill during this time.
The time between the bite and the appearance of symptoms is called the incubation period and it may last for weeks to months. A bite by the animal during the incubation period does not carry a risk of rabies because the virus has not yet made it to the saliva.
2.The Virus Reaches the Brain
Late in the disease, after the virus has reached the brain and multiplied there to cause an inflammation of the brain, it moves from the brain to the salivary glands and saliva.
Also at this time, after the virus has multiplied in the brain, almost all animals begin to show the first signs of rabies. Most of these signs are obvious to even an untrained observer, but within a short period of time, usually within 3 to 5 days, the virus has caused enough damage to the brain that the animal begins to show unmistakable signs of rabies.
Extensive studies on dogs, cats, and ferrets show that the rabies virus can be excreted in the saliva of infected animals several days before illness is apparent. Such extensive studies have not been done for wildlife species but it is known that wildlife species do excrete rabies virus in their saliva before the onset of signs of illness. The excretion of virus may be intermittent, and the relative amount of excreted virus may vary greatly over time, before and after the onset of clinical signs.
The reason there's so much variation in the time between exposure and the onset of the disease is that many factors come into play including the site of the exposure, the type of rabies virus and any immunity in the animal or person exposed.
Reference:http://rabies.emedtv.com/rabies/rabies-transmission.html
From numerous studies conducted on rabid dogs, cats, and ferrets, we know that when the rabies virus is introduced into a muscle through a bite from another animal, it travels from the site of the bite to the brain by moving within nerves. The animal does not appear ill during this time.
The time between the bite and the appearance of symptoms is called the incubation period and it may last for weeks to months. A bite by the animal during the incubation period does not carry a risk of rabies because the virus has not yet made it to the saliva.
2.The Virus Reaches the Brain
Late in the disease, after the virus has reached the brain and multiplied there to cause an inflammation of the brain, it moves from the brain to the salivary glands and saliva.
Also at this time, after the virus has multiplied in the brain, almost all animals begin to show the first signs of rabies. Most of these signs are obvious to even an untrained observer, but within a short period of time, usually within 3 to 5 days, the virus has caused enough damage to the brain that the animal begins to show unmistakable signs of rabies.
Extensive studies on dogs, cats, and ferrets show that the rabies virus can be excreted in the saliva of infected animals several days before illness is apparent. Such extensive studies have not been done for wildlife species but it is known that wildlife species do excrete rabies virus in their saliva before the onset of signs of illness. The excretion of virus may be intermittent, and the relative amount of excreted virus may vary greatly over time, before and after the onset of clinical signs.
The reason there's so much variation in the time between exposure and the onset of the disease is that many factors come into play including the site of the exposure, the type of rabies virus and any immunity in the animal or person exposed.
Reference:http://rabies.emedtv.com/rabies/rabies-transmission.html
The Infectious Path of the Rabies Virus in Raccoon
- Raccoon is bitten by a rabid animal.
- Rabies virus enters the raccoon through infected saliva.
- Rabies virus spreads through the nerves to the spinal cord and brain.
- The virus incubates in raccoon's body for apporximately 3-12 weeks. The raccoon has no signs of illness during this time.
- When it reaches the brain, the virus multiplies rapidly, passes to the salivary glands, and the raccoon begins to show signs of the disease.
- The infected animal usually dies within 7 days of becoming sick.

